Introduction
If you have diabetes, you have an important role in your own medical care, and monitoring your blood sugar is a key part of this.
The major purpose of your diabetes treatment program is to maintain your blood glucose levels within a certain range. The best approach to determine how well your diabetes treatment approach is effective is to check your blood glucose. Fingersticks with a blood glucose meter, or a continuous glucose monitor device, can be used to evaluate blood glucose. Based on blood sugar readings, you can adjust or check the effects of your diet, exercising, diabetes medications, and stress management. Self-monitoring greatly helps in the maintenance of blood glucose (sugar) levels as near to the target as possible in the aspect of diabetes self-management.
Why should you measure blood glucose?
For patients with diabetes mellitus, blood glucose management is a crucial part of case management. The following are some of the benefits of using a continuous glucose monitoring system:
- Determine whether your blood glucose levels are low or high.
- Review how diabetes medications affect your blood sugar levels.
- Check if you are within your blood glucose target range, which would also help you avoid long-term diabetic complications by reducing the severe symptoms of high or low blood glucose levels.
- Understand how your blood glucose level is affected by your food and exercise.
How can I test my blood glucose level?
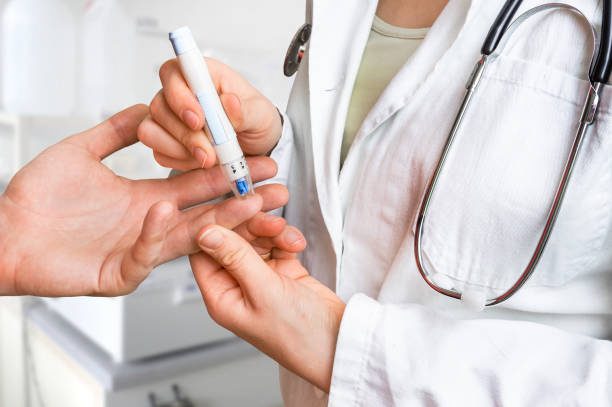
Diabetics can use finger-stick and flash glucose monitoring to keep track of their blood sugar levels. The finger-stick test provides a very simple method to analyze vital nutrients by pricking a finger and taking a small quantity of blood. The blood sample is taken on a test strip without causing any pain or discomfort. The blood sample is collected and then submitted to a laboratory for screening.
While flash glucose monitoring is a modern method of glucose testing that implements sensor reading technology to help assess glucose levels without pricking your finger. It consists of a sensor inserted under your skin to measure blood sugar and a reader that stores glucose readings automatically every minute and records reading every 15 minutes.
Should I consider a Continuous Glucose Meter (CGM)?
Since many people with diabetes are aware of the implications of blood sugar testing in diabetes care management, a continuous glucose monitor(CGM) is a newer technology for diabetic patients that uses a small sensor to constantly re-test blood sugar during the day and night for up to 14 days. CGM reports give you precise information about changes you may use to make day-to-day decisions and discuss with your health care practitioner. CGMs may also automatically gather and send glucose data to a person of your choice, as well as detect dangerous highs and lows so you can stay on track.
CGM systems have been proved to assist patients in maintaining stable blood glucose levels, avoiding episodes of low blood glucose (hypoglycemia) and high blood glucose (hyperglycemia), and lowering the risk of diabetic complications. Unlike regular blood glucose meters, which only give you information for a single instant in time, CGM informs you where your glucose levels are right now, and where they've been.
What are the target blood sugar levels for people with diabetes?
Understanding the ranges of blood sugar levels is an important factor of diabetes self-monitoring. The National Institute for Clinical Excellence (NICE) has offered the following ranges as guidelines, however, each individual's target range should be agreed upon by their doctor or diabetes consultant.
| Target range by type | Upon taking | Before meals | After meals |
| Non-diabetic | 4.0 to 5 mmol/L | Under 7.0 mmol/L | |
| Type 1 Diabetes | 5.0 to 7.0 mmol/L | 4.0 to 7.0 mmol/L | 5.0 to 9.0 mmol/L |
| Type 2 Diabetes | 4.0 to 7.0 mmol/L | Under 8.5 mmol/L | |
| Children with Type 1 Diabetes | 4.0 to 7.0 mmol/L | 4.0 to 7.0 mmol/L | 5.0 to 9.0 mmol/L |
Key time to check your blood sugar
| Recommended Time | Purpose |
| Before Breakfast | This information is helpful in adjusting medicine or long-acting medicine. The Canadian Diabetes Association recommends a fasting blood sugar level of 4.0 to 7.0 mmol/L. |
| 2 hours after meals | This information is helpful in learning how food affects your blood sugar levels. A blood sugar level of 5.0 to 10 mmol/L is recommended by the Canadian Association. |
| At Bedtime | This information is helpful in adjusting diet or diabetic medicine. |
| Before, During, and After exercise | Measuring blood sugar levels before, during, as well as after an exercise can help you see the impact of exercising on your blood sugar levels and help screen for hypoglycemia. |
| Before driving | By checking at this time, you can guarantee that your blood glucose level is within acceptable limits before getting behind the wheel. |
| During stress or illness | Illness or stress may cause your blood glucose to be higher than normal. |
What should I do with the data?
When keeping track of your results, make sure to include the time and date, blood glucose results. Additional notes about what you ate, whether you exercised, any difficulty with illness and stress, medications, and doses you are taking can be helpful. You should discuss your results with your diabetes educator on a frequent basis to determine what they represent and whether you need to make any adjustments to better control your blood sugar.
What should I do if my blood sugar level gets too low or high?
High blood sugar levels or as called hyperglycemia are a major concern that primarily affects people with type 1 or type 2 diabetes. Repeatedly high blood sugar levels can seriously damage your nerves, blood vessels, and organs and produce long-term health-related issues. There are two types of hyperglycemia:
- Fasting hyperglycemia: when blood sugar levels are greater than 7.2 mmol/L after not eating or drinking for at least 8 hours.
- After-meal hyperglycemia: when blood sugar levels are greater than 10.0 mmol/L two hours after eating.
If you notice your blood sugar levels are frequently higher than 10.0 mmol/L, you should drink more water to help remove the excess sugar in your blood through urine and help avoid dehydration. Exercising can also help decrease blood sugar levels, but it can also raise blood sugar levels in some instances, so it's best to see your doctor about what exercise is suitable for you.
Similarly, low blood sugar levels often called as hypoglycemia, occur when blood sugar levels fall below 3.9 mmol/L. A low blood sugar level is serious and should be addressed as soon as possible. When you feel shaky, sweaty, exhausted, have a fast heartbeat, blurred vision, or hunger, you likely have low blood sugar levels. Go for one of the following if you experience one or more of these symptoms:
- Drink one-half cup of fruit juice free from artificial sweeteners because you need to consume about 15 grams of carbohydrates and artificial sweeteners may not provide it.
- Eat 5 or 6 hard candies.
- Eat one tablespoon of sugar, plain or dissolved in water, or eat one tablespoon of honey.
- Chew three glucose tablets.
Then, wait 15 minutes before testing your blood sugar levels again, and repeat until your blood sugar level is 3.9 mmol/L or above. Avoid eating too many sweets, as this can lead to excessive blood sugar and weight gain.
When to see the doctor?
In case of hyperglycemia, see your doctor if you experience any of the following:
- Though taking your diabetic medication, your blood sugar levels remain persistently above 13.3 mmol/L.
- You're sick, and you can't eat or drink anything.
- You have persistent diarrhea or vomiting.
If you have hypoglycemia and your symptoms do not improve after eating a sugary snack, have someone take you to the emergency room or phone your local emergency number; DO NOT drive while your blood sugar is low.
Conclusion
Self-monitoring of blood glucose is a diabetes management tool. Taking readings too frequently or at times other than those suggested, or improperly, may not provide any clinical benefit. Self-monitoring can also be stressful for some people. Because it's crucial to know how often you should monitor your blood glucose, how to interpret the results, what action you should take in response, and how independent you feel about your diabetes, and for that, training is necessary. Mednow virtual care offers a service of consultation with licensed doctors online or over the phone to discuss these issues, help you better understand your blood sugar reading, provides tips for self-testing, and how to reach your glucose target ranges.
This article offers general information only and is not intended as medical or other professional advice. A healthcare provider should be consulted regarding your specific situation. While the information presented is believed to be factual and current, its accuracy is not guaranteed and it should not be regarded as a complete analysis of the subjects discussed. All expressions of opinion reflect the judgement of the authors as of the date of publication and are subject to change. No endorsement of any third parties or their advice, opinions, information, products, or services is expressly given or implied by Mednow or its affiliates.
Commencer